In the high-stakes world of stroke medicine, the mantra is simple and urgent: ‘Time is brain’. Every minute that a major blood clot blocks the flow to the brain, more vital tissue dies. Doctors race against the clock to diagnose, locate the blockage, and intervene. But what if we could give doctors an extra hour in that critical race? A groundbreaking new study suggests we can do exactly that, all thanks to an innovative artificial intelligence imaging tool.
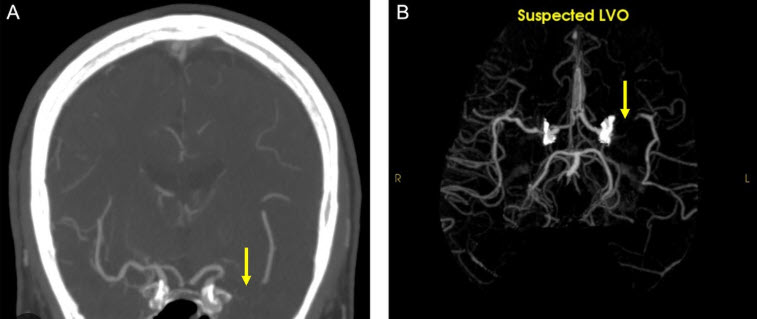
Researchers have found that this sophisticated AI can help doctors spot deadly large vessel occlusions (LVOs);the most severe and debilitating type of stroke-causing clots, an average of more than an hour earlier than current clinical workflows allow.
The AI doesn’t replace the expert eye of a radiologist or neurologist; instead, it acts as an incredibly efficient triage system and second set of eyes. It rapidly processes complex brain scans and immediately flags critical findings, pushing relevant cases to the top of the queue for human review. This efficiency drastically cuts down the time from when a patient arrives at the emergency department to when the critical treatment decision is made…
Earlier diagnosis means faster initiation of life-saving treatments like mechanical thrombectomy (physically removing the clot). The difference between intervention at two hours versus three hours can mean the difference between a patient making a full functional recovery or suffering a severe, lifelong disability.