Even if you have hired the help of a trainer or a therapist to get you started (advised), you must have input towards your own rehabilitation and not be a passive recipient. It’s time for action and knowledge is power. But how do you go about doing this? How do you work with the evidence? Just some thoughts for you to make all this clearer. Firstly, let’s look back at Professor Nick Ward and international colleagues’ ‘agreed definitions’ of the terms ‘rehabilitation’ and ‘recovery’ from 2017. This is worth a couple of screenshots:


See the blue-box? I ask all my students (on online/hybrid courses) to read this out & repeat it with me 3 times. Then we discuss it: it’s important. Definitions really are, otherwise we’re just playing around with words. I then ask them if they think that recovery ever really happens (in near to full totality) for many survivors; which then leads onto more discussion, etc.
Can a generic recovery programme to help you recover be created? For example, is there one ‘programme’ that will fit everyone? It would be much easier that way but the most accepted answer is ‘no’. I’m afraid not. You need something highly customised and evidence based (and you are a changing target, remember, so any ‘programme’ must allow you to work on the edges of your current ability, with progressions that you can only try/experiment with once you gain some success (so progressions can’t in any way be ‘pre-set’, but become part of recovery).
The good news for you is that it’s practically certain that there are numerous things that most or ALL stroke survivors must do to get/regain the above. You can start with basic tasks that you need to master in order that you can work towards more complex tasks. You will ‘get nothing by doing nothing’.
To boil it down (black and white style), you may well need to countenance attempting these 10 things below, over time. It’s a great ‘starter for 10’ way to look at the totality of recovery:
- Understand how to produce, start, a very manageable, customised self-rehab programme (with the assistance of a physio or specialist neuro-rehab ARNI instructor).
- Understand what, when and why you’re doing what you’re doing, instead of doing things ‘piece-meal’. You need your progress trajectory to be upwards.
- Understand what factors you can play with, try out, evaluate and combine interventions (how to manipulate the concepts, principles and available adjuncts/interventions).
- How to record & evaluate: the no. 2 of 2 of re-training. No. 1 is starting it and doing it.
- Understand that specific goals will only come once you can see your way (ie, get some successes under your belt, which is why learning how to get down and up from the floor with no help or support is incredibly important). Many people, having been told they need to goal-set, don’t then build in the try/fail factor – and get annoyed/stop trying to self-rehab and/or engage with a physio or trainer on a weekly basis. Which isn’t good.
- Understand how to, and initiate, weight-bearing, balance, co-ordination, postural and gait control over time.
- Understand how to, and initiate, the decrease of upper limb spasticity/flaccidity if you have it & increase functional movement return over time.
- Understand how to, and initiate, the increase of muscular, tendon, ligament and bone strength over time.
- Understand how to, and initiate the increase of confidence and removal of the the fear of the consequences of exercising.
- Understand how to become progressively more self-sufficient, make tremendous efforts to get that way, giving hope to those who love and care for you & then become productive in an occupation and/or hobby be happy with life and give back to others.
Can I do these things? ABSOLUTELY!! These can all be achieved by you, to a certain degree, however old you are, step by step, if you’re motivated and are prepared to sacrifice time and effort (again, if you are able to/if appropriate).
 Can I recover from stroke if I can’t find anyone to help me? ABSOLUTELY! You can still self-rehab very successfully indeed, but to start, you’ll appreciate that knowledge is power. Which is why therapists and specialists instructors are well worth ‘using’, as they can provide you with the grounding that you probably need to understand how to reach ‘stages’, get to stages, make your own stages etc. And you need to do your knowledge accumulation (if you can.. ). And again, you need to know (quickly), how to avoid reaching out to tenuous/non-evidence based sources or for interventions out there with little to no evidence for efficacy. Or those which seem to show efficacy but in examination, have perhaps manage this by apparent strong relationships with/to those with good evidence for efficacy. You’ll invariably end up wasting money and time ingesting metaphorical snake-oil.
Can I recover from stroke if I can’t find anyone to help me? ABSOLUTELY! You can still self-rehab very successfully indeed, but to start, you’ll appreciate that knowledge is power. Which is why therapists and specialists instructors are well worth ‘using’, as they can provide you with the grounding that you probably need to understand how to reach ‘stages’, get to stages, make your own stages etc. And you need to do your knowledge accumulation (if you can.. ). And again, you need to know (quickly), how to avoid reaching out to tenuous/non-evidence based sources or for interventions out there with little to no evidence for efficacy. Or those which seem to show efficacy but in examination, have perhaps manage this by apparent strong relationships with/to those with good evidence for efficacy. You’ll invariably end up wasting money and time ingesting metaphorical snake-oil.
What sources can I look at to get started? Well, you could start by have a read of Had a Stroke? Now What? to get you started… click the book cover or press here. I’ve done my best in 244 pages of the neurorehabilitation evidence-base, 25 years of experience as a survivor and help from the numerous worldwide experts in stroke I’m lucky enough to be supported by/linked with, to provide you with the best picture of ‘what to try/do/what perhaps to avoid’. This book gives lots of indicators concerning the evidence applicable for your situation right now. It also shows lots more paths (many via the 3rd Sector like ARNI, concerning how you can ask people out there to send you links/clips/sites to help you get more acquainted in the importance of the evidence…

What is the ‘evidence’ for recovery after stroke? Basically, you need to try understand the parameters of your recovery. Ie; ‘understand it, do it’. Or in practice, ‘start, make efforts, gain best understanding as you can over time, and build on your know-how constantly’. In a word, you’ve got to be intensely INTERESTED. No way you should just let yourself become a passive recipient of things happening to you (or not).
Of the many, excellent overall meta-analyses that exist, the regularly updated Evidence-Based Review of Stroke Rehabilitation (Professor Robert Teasell’s team in Ontario) is one of my ‘go to’ ones. It’s an in-depth reviews of well over 4,500 studies including over 2,170 randomized controlled trials, with ‘lay-summaries’ that are very useful indeed to further your understanding whoever you are, once you’ve understood the terminology. So, for you too, there’s no reason it can’t help to guide the parameters of what you’re now ‘dealing with’.
Will I need help to understand what ‘the evidence’ is? It’s difficult for the majority of stroke survivors to do, which is why instructors and physios (who are applying the current evidence) are so very necessary. The Reviews are for clinicians & therapists mainly for this reason. But, as above, there’s no reason why family members/carers/friends can’t start to investigate the evidence and start to learn from it. Understanding the nuances of the evidence and exactly why various interventions can change from, for example, ‘strong’ to ‘mixed evidence for’, or, the nuanced word ‘may be’… (beneficial) that seems to have crept into these reviews.
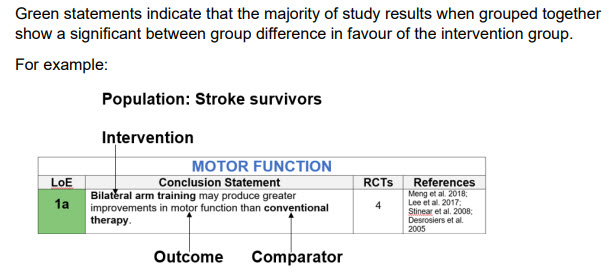
For example: the upper extremity interventions section (2020) shows the interventions and their applications, with very useful summaries of their efficacies with:

So, for example, you may be recommended ‘task-training’ to do. But why? And how can you practically set it up, do it? And what in real terms will it do for you? And how to optimise its effectiveness….
Nevertheless, as a template of what to do and what not to do, if you get to understand the terms (get a copy of ‘Had a Stroke, Now What’ and use the ‘Terminology’ pages in the introduction) and can interpret how to practically create ‘task-specific training’ for yourself.
Also, you could go on to the ARNI site and see ‘task-board’ in products section as example or just make a similar one instructions on one of the any-time stream (vid 6 of 7) via log-in to your device – click the picture or here ).
You can see that you need over time to become the ‘patient-professional’. Or have someone close to you (family member/carer/friend) who can help you in this regard/do it for you. In short, you/they need to get to understand , reasonably quickly, what the current evidence recommends, doesn’t recommend and what it concludes about the efficacies of various interventions.
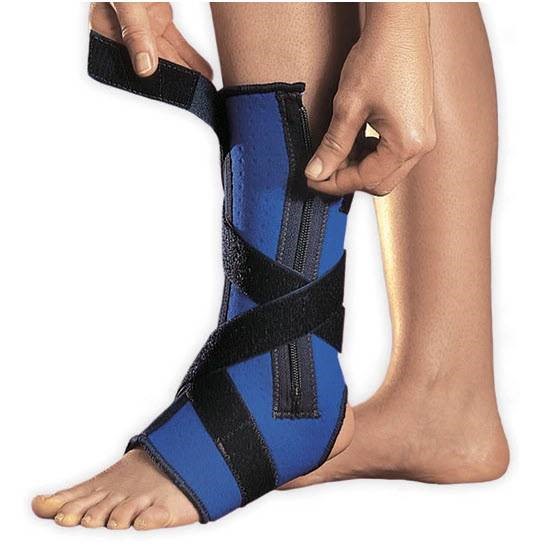
A further (random) example: therapists often use/recommend splinting and orthoses with patients. But why? What are they hoping to achieve? Do you know? If not, then having a look at conclusions of the current evidence about the intervention is useful: see screenshot below.
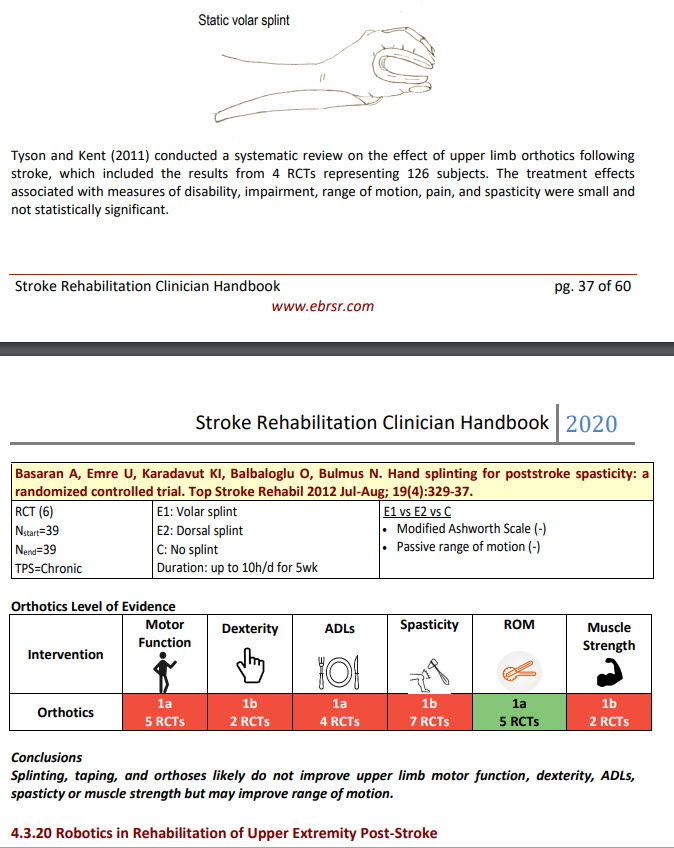 The ‘sum of the evidence-base’ is the best we have to work with – it’s often a little out of date due to many factors, not least the nature of the time it takes to collate and display. But it’s being updated all the time. Also (I’ve found), there are very many very friendly experts in Universities who may certainly be approached in the right manner with a question or two, who will be able to refer you to online resources that may be appropriate to aid your further understanding. Ask me, if you like, and I may be able to help by asking a colleague researching in the area of your question.
The ‘sum of the evidence-base’ is the best we have to work with – it’s often a little out of date due to many factors, not least the nature of the time it takes to collate and display. But it’s being updated all the time. Also (I’ve found), there are very many very friendly experts in Universities who may certainly be approached in the right manner with a question or two, who will be able to refer you to online resources that may be appropriate to aid your further understanding. Ask me, if you like, and I may be able to help by asking a colleague researching in the area of your question.
 In short, as above, you need to try and understand the parameters of what you’re dealing with. This is something for when you’re now home or in other accommodation, such as your circumstances dictate.
In short, as above, you need to try and understand the parameters of what you’re dealing with. This is something for when you’re now home or in other accommodation, such as your circumstances dictate.
So, I hope to emphasise to you with this post that the evidence can aid you not to waste lots of time and money and concentrate on the regain of your functional movement action control as much as you can, learning essential physical coping strategies which are highly individual, relying as they do on your own genetics, status of accompanying medical problems, attitude (drive, persistence, desire and motivation) and so very many other factors.
The longer you’re a stroke survivor, the more you’ll notice that you can ‘win’ or control (manage) many of these but others will have to be accepted. And, I have to tell you, that re-training efforts can never stop, throughout the rest of your life. Sounds like bad news?! Not so… I’ll show why, in a forthcoming post.
Long term stroke survivors reading this will be nodding to themselves. Newer stroke survivors will get to understand what I mean. The good news is that: ‘retraining’ can (and should) very soon phase into an enjoyable and social physical activity wherein you are actively rehabilitating. The reason is that formal re-training is essentially boring. We all know it. Why should it be exciting? It’s grind! So you’ve GOT to find a way to make ‘it’ part of your everyday life. So now you see that you’ve got to find the combination of ‘its’ that seem to work best to tackle your limitations (by challenging yourself at the edges of your current ability).
 If this sounds abstract, here’s a simple formula as a starter for 10.
If this sounds abstract, here’s a simple formula as a starter for 10.
Regular formal rehab + everyday re-training efforts split into a number of aspects + about 3 hobbies which all challenge your limitations (there are quite a few to try; it just takes trying trying a many things as you can think of + try and have as much fun as possible + try and make ‘yourself’ and your own recovery (remember the definition above?!) an experiment: go beyond that which anyone thought possible of you.
Find out exactly how I did these three things in the Successful Stroke Survivor (click picture of book or here).
And lastly (encouragingly), it seems that ‘formal training’ is finite… it must be. But it must be done ‘right’ so you can phase into a maintaining status quo in some areas if there’s absolutely no other option – and regularly improve/know how to regain where you were in others (usually micro-improvements) via re-training.
Get in touch with ARNI Stroke Rehab Charity now if you think we can help you. Call Us : 0203 053 0111





 Each year there are more than 100,000 first-time strokes in the UK; and as you may have heard on the news a couple of weeks ago, this number is set to rise by 50% by 2035.
Each year there are more than 100,000 first-time strokes in the UK; and as you may have heard on the news a couple of weeks ago, this number is set to rise by 50% by 2035. 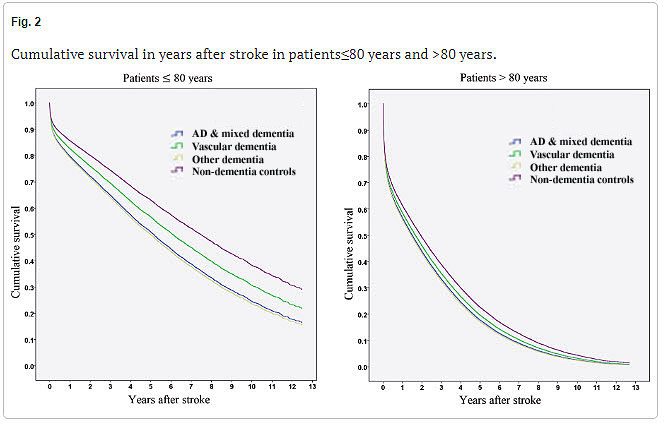

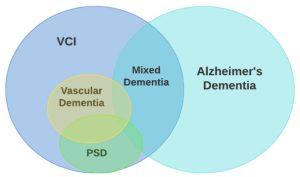
 struggling with memory issues, who may find music therapeutic and relaxing. It lets users play the piano, even if they haven’t played it in years (or ever), for free. With a library of thousands of songs, people with Alzheimer’s and dementia can use the app to access old favourite songs and unlock good memories in the process.
struggling with memory issues, who may find music therapeutic and relaxing. It lets users play the piano, even if they haven’t played it in years (or ever), for free. With a library of thousands of songs, people with Alzheimer’s and dementia can use the app to access old favourite songs and unlock good memories in the process.

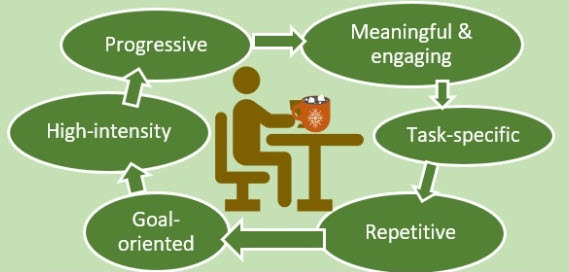 So, overall, whether using an assistive device or not when doing re-training, ‘task-practice’ is pretty much necessary/required.
So, overall, whether using an assistive device or not when doing re-training, ‘task-practice’ is pretty much necessary/required.  Task training is critical because it will ‘force’ you to practice using your more-affected limb. This is why the Evidence-Based Review of Stroke Rehabilitation (EBRSR) concludes that constraint induced movement therapy (CIMT) in clinical settings, for those who meet the qualifying criteria, shows strong evidence of benefit in comparison to traditional therapies in the chronic stage of stroke. CIMT is a great example of task training for the upper-limb. 30 to 66 % of stroke survivors report no longer being able to use the affected arm despite trying to rehabilitate and are in danger of avoiding using it (‘learned non-use’ or inattention/ neglect of the limb). Several factors might explain this phenomenon. First, you may see no reason to try and use your bad arm and therefore remain ignorant of underlying motor potential. Second, you may not know how to use any emerging isolated movement for functional performance.
Task training is critical because it will ‘force’ you to practice using your more-affected limb. This is why the Evidence-Based Review of Stroke Rehabilitation (EBRSR) concludes that constraint induced movement therapy (CIMT) in clinical settings, for those who meet the qualifying criteria, shows strong evidence of benefit in comparison to traditional therapies in the chronic stage of stroke. CIMT is a great example of task training for the upper-limb. 30 to 66 % of stroke survivors report no longer being able to use the affected arm despite trying to rehabilitate and are in danger of avoiding using it (‘learned non-use’ or inattention/ neglect of the limb). Several factors might explain this phenomenon. First, you may see no reason to try and use your bad arm and therefore remain ignorant of underlying motor potential. Second, you may not know how to use any emerging isolated movement for functional performance.
 One great example: I created ‘DJ-Therapy’ to get my upper limb working again. I basically made up a hugely successful paradigm which was suitable for me. How I did it is all listed in
One great example: I created ‘DJ-Therapy’ to get my upper limb working again. I basically made up a hugely successful paradigm which was suitable for me. How I did it is all listed in 





 Virtual reality (VR) basically means interactive simulations of activities within environments that appear and feel similar to real-world objects and events (augmented reality).
Virtual reality (VR) basically means interactive simulations of activities within environments that appear and feel similar to real-world objects and events (augmented reality). VR interventions can be expensive but most are usually created to be affordable. A set-up often features just a keyboard, a mouse, a specialised multi-modal device such as a console or gloves with built-in movement sensors. Haptic devices are a good example of this. VR devices often provide feedback on movement execution and goal attainment. Many will help you to repetitively practice large and small movement-based tasks through the use of fun and motivating activities that can be completed while sitting, standing or lying.
VR interventions can be expensive but most are usually created to be affordable. A set-up often features just a keyboard, a mouse, a specialised multi-modal device such as a console or gloves with built-in movement sensors. Haptic devices are a good example of this. VR devices often provide feedback on movement execution and goal attainment. Many will help you to repetitively practice large and small movement-based tasks through the use of fun and motivating activities that can be completed while sitting, standing or lying. A
A 



 Another
Another  The analysis was limited in many ways: for example. the highest number of studies conducted to date have been in Asia, Europe, and North America, and no studies have been reported from Africa, South America, and Australia, so this problem adversely affected the generalisability of the study results. Nevertheless, the results of this large-scale meta-analysis show that, compared to the elderly who did not receive the flu vaccine,
The analysis was limited in many ways: for example. the highest number of studies conducted to date have been in Asia, Europe, and North America, and no studies have been reported from Africa, South America, and Australia, so this problem adversely affected the generalisability of the study results. Nevertheless, the results of this large-scale meta-analysis show that, compared to the elderly who did not receive the flu vaccine,

 The Department of Computing at Imperial College London is evaluating a platform called ‘CogiGames Home’, and have asked ARNI Charity to pass this message below to stroke survivors, carers (and professionals to forward if appropriate):
The Department of Computing at Imperial College London is evaluating a platform called ‘CogiGames Home’, and have asked ARNI Charity to pass this message below to stroke survivors, carers (and professionals to forward if appropriate): 




 Balance (both standing and walking) training is the only effective treatment for balance disorders, as recommended by the National Institute for Health and Care Excellence (NICE) UK
Balance (both standing and walking) training is the only effective treatment for balance disorders, as recommended by the National Institute for Health and Care Excellence (NICE) UK At University College London’s Institute of Neurology, a large-scale global research project (funded by a European Union Horizon 2021 grant), is under way (led by
At University College London’s Institute of Neurology, a large-scale global research project (funded by a European Union Horizon 2021 grant), is under way (led by 
