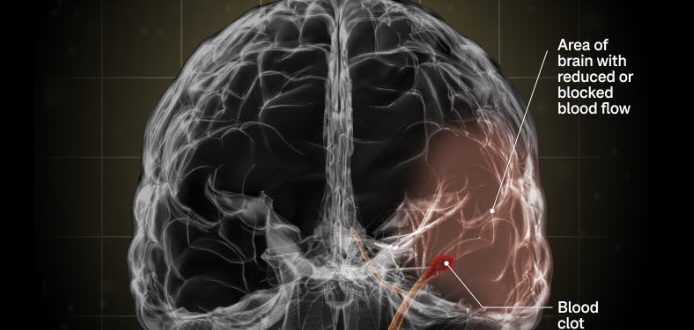
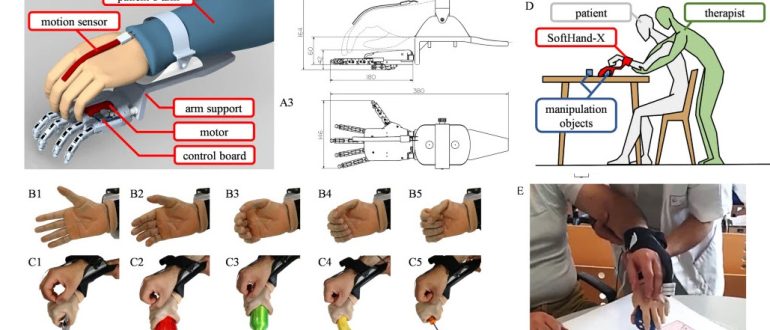
Research continues to validate the effectiveness of advanced wearable technology, like the Neofect Smart Glove for upper-limb rehab. Smart Glove is a San Fran-based high-tech stroke rehab product for your hand that follows your hand motions, measuring the slightest movements in your hand with accelerometer and bending sensors while performing gamified exercises.
A recent study published in the Journal of NeuroEngineering and Rehabilitation showed significant functional gains for patients using the glove alongside conventional therapy compared to conventional therapy alone. It proved a motivating way to perform progressive hand exercises at home.
The Smart Glove uses engaging, game-based virtual reality to provide high-repetition, task-specific practice, a crucial component for inducing neuroplasticity. Integrated sensors monitor individual finger and wrist movements, giving patients and clinicians real-time feedback and objective tracking data on progress.
Functional near-infrared spectroscopy (fNIRS) analysis demonstrates increased brain activity in the motor cortex during Smart Glove training, providing objective evidence of cortical reorganisation. Patients showed statistically significant improvements in standardised tests of hand function (e.g., Fugl-Meyer Assessment and Jebsen-Taylor Hand Function Test).
This tech for stroke seems to offer a promising tool for increasing a survivor’s motivation and extending rehabilitation beyond the clinic; hopefully accelerating recoveries and improving the quality of survivors’ lives.